Guidelines and Consensus | Expert Consensus on Transvaginal Sacrospinous Ligament Fixation (2025 Edition)
Pelvic organ prolapse (POP) is a common female pelvic floor dysfunction disorder characterized by the descent of pelvic organs (such as the uterus, bladder, or rectum) below their normal anatomical position due to weakness or damage of the supportive tissues. Apical prolapse mostly refers to the descent of the uterus (cervix) or the vaginal vault (after hysterectomy). These patients often present with concurrent anterior and posterior vaginal wall prolapse. After apical restoration, approximately 50% of anterior vaginal wall prolapse and 30% of posterior vaginal wall prolapse can be corrected.
After more than 60 years of development and practice, sacrospinous ligament fixation (SSLF) has been proven to be a safe and effective procedure and is recommended as one of the primary surgical options for treating apical prolapse in multiple clinical guidelines. SSLF restores Level I support by fixing the apex to the sacrospinous ligament (SSL). It can be performed via abdominal, vaginal, or laparoscopic routes, with the vaginal route being the most common. To standardize its application and promote its adoption, the Gynecological Vaginal Surgery Professional Committee of the China Maternal and Child Health Association organized domestic pelvic floor experts to discuss and formulate this consensus, aiming to provide clinical advice and reference for this technique. Obstetrics and Gynecology Online has compiled the key points as follows for the benefit of readers.
1. Key Clinical Anatomy Points for Sacrospinous Ligament Fixation
1.1 Anatomical Points
The SSL is composed of dense connective tissue, distributed from the first transverse process of the coccyx and the lateral border of the fourth sacral foramen to the ischial spine. It runs in the same direction as the coccygeus muscle, together forming the coccygeus-sacrospinous ligament complex (C-SSL). It is fixed in position and has strong tensile strength, making it suitable for anchoring and suspension in pelvic floor reconstruction surgery.
1.2 Adjacent Nerves and Vessels
The SSL region is rich in nerves and blood vessels, including the pudendal nerve, sacral nerves, sciatic nerve, and internal pudendal artery. Anatomical studies show that the fourth sacral nerve runs obliquely upward and outward on the medial one-third surface of the SSL, joining the second and third sacral nerves to form the pudendal nerve, which is mostly located along the superior border of the lateral one-third of the SSL. The average distance between the sacral nerve and the superior border of the SSL is 0.7 cm, and they may sometimes be in close contact. The nerves to the coccygeus and levator ani muscles are located in the lateral one-third of the SSL. After branching from the internal iliac artery, the internal pudendal artery passes behind the SSL, around the ischial spine, and exits the pelvis through the greater sciatic foramen. The inferior gluteal artery exits the pelvis between the second and third or first and second sacral nerves. See Figure 1. The surgical approach for SSLF via the posterior vaginal wall sequentially dissects the rectovaginal space and the pararectal space, which is relatively safe and less likely to injure important neurovascular structures.
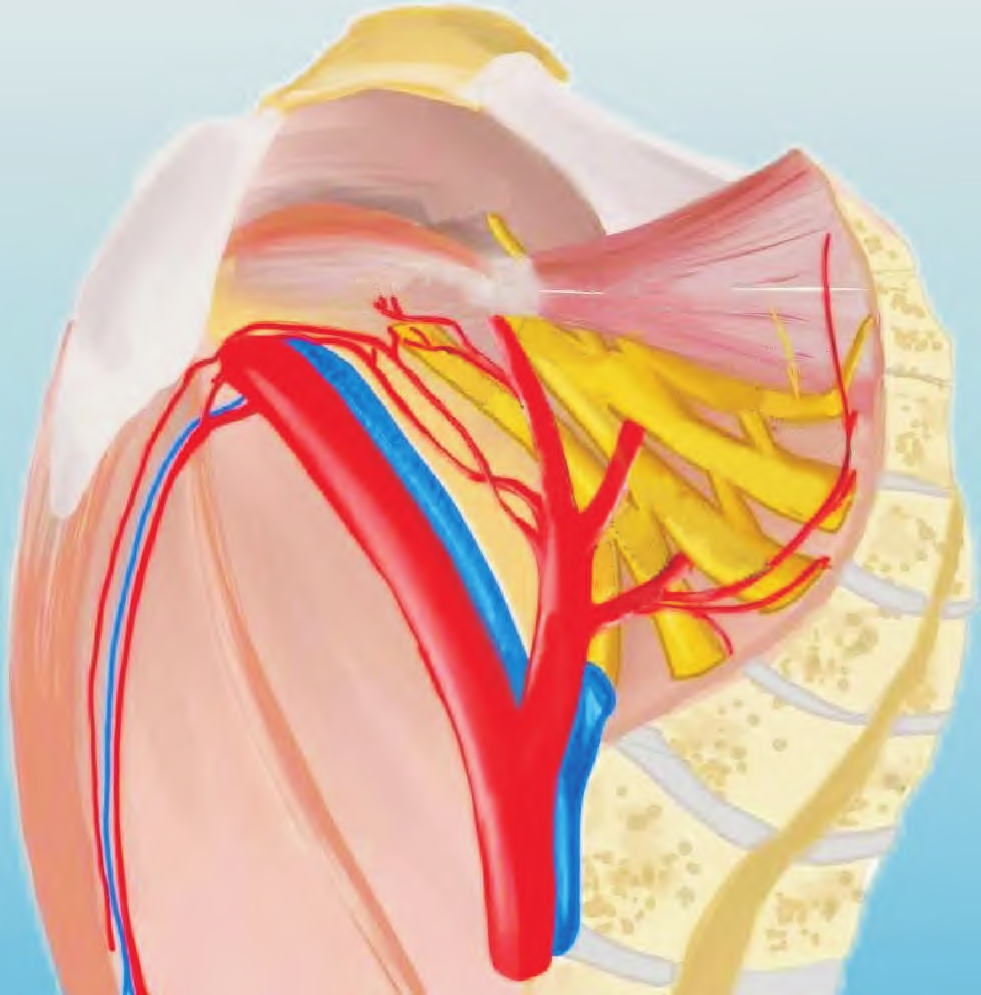
Figure 1 Anatomical diagram of SSL (right sagittal view, drawn by Foshan Women and Children’s Hospital)
1.3 Optimal Anchoring Point
Recommendation: The optimal anchoring point for SSLF is 1.5–3.0 cm medial to the ischial spine, corresponding to the middle one-third of the C-SSL, without exceeding the superior border and without penetrating the full thickness (Recommendation level: Class 2A).
2. Indications and Contraindications
2.1 Indications
The “Chinese Guidelines for Diagnosis and Treatment of Pelvic Organ Prolapse (2020 Edition)” clearly states that SSLF is primarily indicated for symptomatic patients with predominant middle-compartment defects and Pelvic Organ Prolapse Quantification (POP-Q) stage ≥ II.
2.2 Contraindications
Contraindications for SSLF include active genital tract infections such as vaginitis and vaginal mucosal ulcers; anatomical abnormalities of the pelvic floor such as vaginal stenosis, short vagina, pelvic deformities, or hip prosthesis; and severe medical comorbidities precluding surgery.
Recommendation: SSLF is primarily indicated for symptomatic patients with predominant middle-compartment defects and POP-Q stage ≥ II (Recommendation level: Class 2A).
3. Preoperative Evaluation
Assess symptoms, obtain medical history, evaluate the type and degree of prolapse based on the “compartment theory” and the “three-level support theory,” and clarify treatment goals. Use questionnaires such as PFIQ-7 and PISQ to assess urinary, bowel symptoms, and sexual function. Record the degree of prolapse using the POP-Q scoring system preoperatively, and examine each vaginal wall with a bivalve speculum. Assess occult urinary incontinence and pelvic floor muscle tone after reducing the prolapse. Preoperative post-void residual measurement, urodynamic studies, voiding diaries, and pad tests help determine the type of urinary incontinence. Pelvic floor ultrasound and MRI provide additional information for complex cases.
Recommendation: A comprehensive preoperative history should be obtained to clarify the type and degree of prolapse, and appropriate ancillary tests should be selected based on local resources and case complexity (Recommendation level: Class 2A).
4. Surgical Steps and Key Points
This consensus uses right-sided SSLF via the posterior vaginal wall (with hysterectomy) as an example for illustration, following the principle of “lateral dissection, midline suturing”.
4.1 Positioning: Dorsal lithotomy position.
4.2 Incision selection and creation
A longitudinal midline incision or an incision 1 cm to the right of the midline on the posterior vaginal wall, approximately 2–3 cm from the hymenal ring and the vaginal apex. Hydrodissection can be used to assist separation.
4.3 Dissection of the rectovaginal space and the right pararectal space
Incise the posterior vaginal wall full-thickness. Sharply and bluntly dissect the rectovaginal space to the right. Sharply and bluntly dissect the right pararectal space towards the ischial spine. After palpating and identifying the right ischial spine, dissect the peritoneal sac on the ventral side of the SSL towards the sacrococcygeal direction, enlarging the right pararectal space sufficiently to insert a vaginal retractor.
4.4 Exposure of the SSL
Use a retractor to depress the rectum, push the peritoneal sac medially and upward, and dissect the membranous connective tissue overlying the SSL to expose the SSL.
4.5 Identification of the anchoring point
Under direct visualization, use a dedicated suturing device/needle holder to place the first and second anchoring sutures in the middle one-third of the SSL (1.5–3.0 cm medial to the ischial spine), with approximately 1 cm between the two sutures. Pull the sutures to confirm their strength. Some surgeons perform suture placement by palpating with a finger, but a digital rectal examination is necessary to rule out rectal injury. Several suturing techniques: ① Do not exceed the superior border of the SSL or penetrate its full thickness; ② Insert the needle perpendicular to the SSL to reduce the likelihood of nerve entrapment; ③ Use oblique suturing when the SSL is relatively thin to reduce tension and avoid ligament tearing.
4.6 Suturing and fixation of the apex
Extend the incision towards the vaginal apex. Suture and anchor the two sutures to the vaginal apex at the level of the farthest attachment point of the uterosacral-cardinal ligament complex on the apex. Alternatively, fix the two sutures to the farthest points of the uterosacral-cardinal ligament complex on both sides. For patients retaining the uterus and/or cervix, the sutures can be fixed to the cervical fascia (at the level of the farthest point of the uterosacral-cardinal ligament complex).
4.7 Closure of the vaginal incision
Use 2-0 absorbable suture to continuously close the upper part of the vaginal incision starting from the vaginal apex. All non-absorbable sutures at the apex must be buried to prevent suture exposure.
4.8 Tying knots and repositioning the vagina
Tie the knots at the apex to reposition and fix the vaginal apex to the SSL, avoiding any suture bridge between them.
4.9 Closure of the lower part of the vaginal incision
Re-check for bleeding. Place a drain if necessary.
5. Management and Prevention of Complications
5.1 Buttock or posterior thigh pain
The incidence of nerve injury after SSLF is 3%–15%, mostly due to entrapment of branches of the pudendal nerve, such as the levator ani nerve, manifesting as pain in the buttock and posterior thigh. Rarely, the sciatic nerve may be entrapped. If the straight leg raise test is positive, with severe persistent buttock and lower extremity pain and motor dysfunction, early evaluation and suture removal are necessary to avoid permanent nerve damage.
Recommendation: Post-SSLF pain usually resolves within 4–6 weeks. In severe cases, sutures should be removed promptly (Recommendation level: Class 2A).
5.2 Bleeding and risk of pelvic hematoma
The risk of life-threatening bleeding during SSLF is 0.2%–2%. Most bleeding can be effectively controlled within 5–10 minutes using hemostatic agents and vaginal packing. If conservative measures fail, vascular interventional embolization should be considered. The incidence of postoperative pelvic hematoma is approximately 2.6%, often due to inadequate compression hemostasis or poor drainage. Asymptomatic small pelvic hematomas often resolve spontaneously without special treatment, usually healing within 3–6 months. If the hematoma is not enlarging, conservative observation is appropriate; if it continues to enlarge, evacuation of the hematoma, hemostasis, and drain placement are required. If the hematoma induces infection or intestinal obstruction, reoperation is needed.
Recommendation: Methods to control bleeding include compression hemostasis, direct suture ligation, vaginal packing, and vascular interventional embolization. A continuously enlarging hematoma requires evacuation, hemostasis, and drain placement (Recommendation level: Class 2A).
5.3 Rectal or bladder injury
Recommendation: Promptly identify and repair injuries to adjacent organs, seeking surgical assistance for repair if necessary (Recommendation level: Class 2B).
5.4 Infection
The postoperative wound infection rate after SSLF is approximately 3.7%, mainly associated with bleeding and pelvic hematoma.
Recommendation: Routine use of prophylactic antibiotics is recommended (Recommendation level: Class 2B).
5.5 Suture exposure
The suture exposure rate after SSLF is 3.0%–8.6%, presenting as mild vaginal bleeding, increased discharge, or exposed sutures and polyp formation. The use of 1-0 non-absorbable sutures is recommended, but this may increase the risk of suture erosion and granuloma formation. Sutures exposed for more than six months should be trimmed. Some studies use PDS II delayed-absorbable sutures to reduce exposure risk.
Recommendation: Routine postoperative follow-up should be performed to check apical healing and suture exposure (Recommendation level: Class 2A).
5.6 Risk of postoperative anterior vaginal wall prolapse
Recommendation: Concurrent anterior compartment prolapse should be corrected intraoperatively, and attention should be paid to preventing postoperative anterior compartment prolapse (Recommendation level: Class 2A).
5.7 Recurrence of apical prolapse after surgery
Recommendation: Recurrence of apical prolapse after surgery mainly occurs within the first postoperative year. It is recommended to use two sutures for anchoring during the procedure and to provide adequate patient education postoperatively (Recommendation level: Class 2A).
6. Surgical Evolution, Developments, and Controversial Points
6.1 Recommendation for unilateral or bilateral SSLF
SSLF is typically performed unilaterally. For some patients with stage III–IV apical prolapse or combined multi-compartment defects, bilateral SSLF may be considered if there is adequate vaginal length and width.
Recommendation: SSLF is usually unilateral. Bilateral SSLF is applicable for selected cases with stage III–IV apical prolapse or combined multi-compartment defects and adequate vaginal length and width (Recommendation level: Class 2A).
6.2 Opinions on uterine preservation versus removal
Uterine prolapse is primarily caused by a defect in Level I support, not prolapse of the uterus itself. Therefore, hysterectomy should not be considered a mandatory procedure for pelvic floor reconstruction. After excluding uterine and cervical pathology, and considering the patient’s preference, uterus-preserving SSLF is safe and feasible.
Recommendation: After excluding uterine and cervical pathology, uterus-preserving SSLF does not affect long-term subjective and objective cure rates (Recommendation level: Class 2A).
6.3 Anterior vaginal wall approach
Recommendation: The appropriate surgical approach should be selected based on concomitant prolapse of other compartments, surgeon’s expertise, and available instruments (Recommendation level: Class 2B).
6.4 Transvaginal endoscopic technique
Recommendation: The transvaginal endoscopic technique offers advantages in visualization, but current evidence-based medical evidence is limited (Recommendation level: Class 2B).
In summary, this consensus integrates domestic and international research findings, combining evidence levels with expert opinions to propose reference recommendations for standardizing the clinical application of SSLF. However, these recommendations are not absolute for all clinical situations. Physicians should formulate treatment plans together with patients based on the patient’s actual condition and individual needs.
Clinical Study: Finite Element Analysis of TVT and TVT-O at Different Positions for Treating Stress Urinary Incontinence in Elderly Women
Guideline Consensus | "Expert Consensus on the Individualized Optimized Diagnosis and Treatment Technology System for Pelvic Floor Dysfunction in Elderly Women" (2024)

