Pelvic Floor Literature Express | Global Trends and Future Projections of Pelvic Organ Prolapse: A 30-Year Epidemiological Study
To keep abreast of international academic developments and promote the exchange of pelvic floor diagnosis and treatment experience, the Pelvic Floor Team of the Department of Gynecology, International Peace Maternity and Child Health Hospital, Shanghai Jiao Tong University School of Medicine, has compiled a summary of literature reviews. This summary covers the latest important literature and conference updates in the pelvic floor field both domestically and internationally, and we look forward to learning and discussing together with colleagues in pelvic floor medicine for mutual improvement.
Literature of the Issue
Global Trends in Prevalence and Future Projections of Pelvic Organ Prolapse: A 30-Year Epidemiological Study
This week we bring you a very important paper. This study, based on data from the Global Burden of Disease database, describes the trends in the incidence of pelvic organ prolapse across different regions of the world over the past 30 years.
Compiled by: Chu Lei
Reviewed by: Liu Ping
Global Trends in Prevalence and Future Projections of Pelvic Organ Prolapse: A 30-year Epidemiological Study
Global Trends in Prevalence and Future Projections of Pelvic Organ Prolapse: A 30‑year Epidemiological Study
Li P, et al. Int Urogynecol J. 2025 Jan 21.
Chinese-English Glossary:
SDI: Socio-demographic Index
BAPC: Bayesian age-period-cohort model
ASPR: Age-standardized prevalence rate
YLD: Years lived with disability
GBD: Global Burden of Disease
Introduction
Pelvic organ prolapse (POP) is a prevalent condition among women. Despite its high prevalence, comprehensive global studies are lacking, underscoring the urgent need for tailored prevention and treatment strategies. This study aims to examine the global burden of POP from 1990 to 2021 and predict future trends using GBD data.
Methods
Data were sourced from the GBD 2021 database. The Bayesian age-period-cohort (BAPC) model was used to analyze trends and predict future burden, with age-standardized prevalence rate (ASPR) and years lived with disability (YLD) as key metrics.
Results
Global POP burden and stratification by Socio-demographic Index level
Globally, the number of POP cases increased from 73.73 million (95% UI 61.15–87.99) in 1990 to 124.37 million (95% UI 103.4–148.05) in 2021, a rise of 68.68%. In 1990, the age-standardized prevalence rate of POP was 3373.9 per 100,000 (95% UI 2787.7–4014.5), and in 2021 it was 2769.4 per 100,000 (95% UI 2299.2–3298.2), a decrease of 17.9%. Over the past three decades, global annual YLDs related to POP increased by 40%, from 226,760 (95% UI 110,697–433,084) in 1990 to 380,599 (95% UI 182,691–722,489) in 2021. From 1990 to 2021, the age-standardized YLD rate decreased from 10.4 per 100,000 (95% UI 5–19.6) to 8.5 per 100,000 (95% UI 4.1–16.2), similar to the trend in ASPR, a decline of 18.1%.
Stratification by Socio-demographic Index level showed that the burden of age-standardized prevalence of POP was lowest in high SDI regions and highest in low SDI regions (Figure 1A). In 2021, the highest age-standardized prevalence was in low SDI regions at 4110.8/100,000, while the lowest was in high-middle SDI regions at 2101.3/100,000. Compared to 1990, age-standardized prevalence decreased across all SDI regions, with the largest decline in low-middle SDI regions (−35.6%, 95% UI −37.1% to −34.3%). From 1990 to 2021, low SDI regions experienced the highest age-standardized YLD burden due to POP at 12.6 per 100,000, while high SDI regions had the lowest at 6.4 per 100,000. These findings are consistent with ASPR estimates (Figure 1B). Since 1990, age-standardized YLD rates have declined in all five SDI regions, with the greatest decrease in low-middle SDI regions (−35.6%, 95% UI −37.1% to −34.3%).
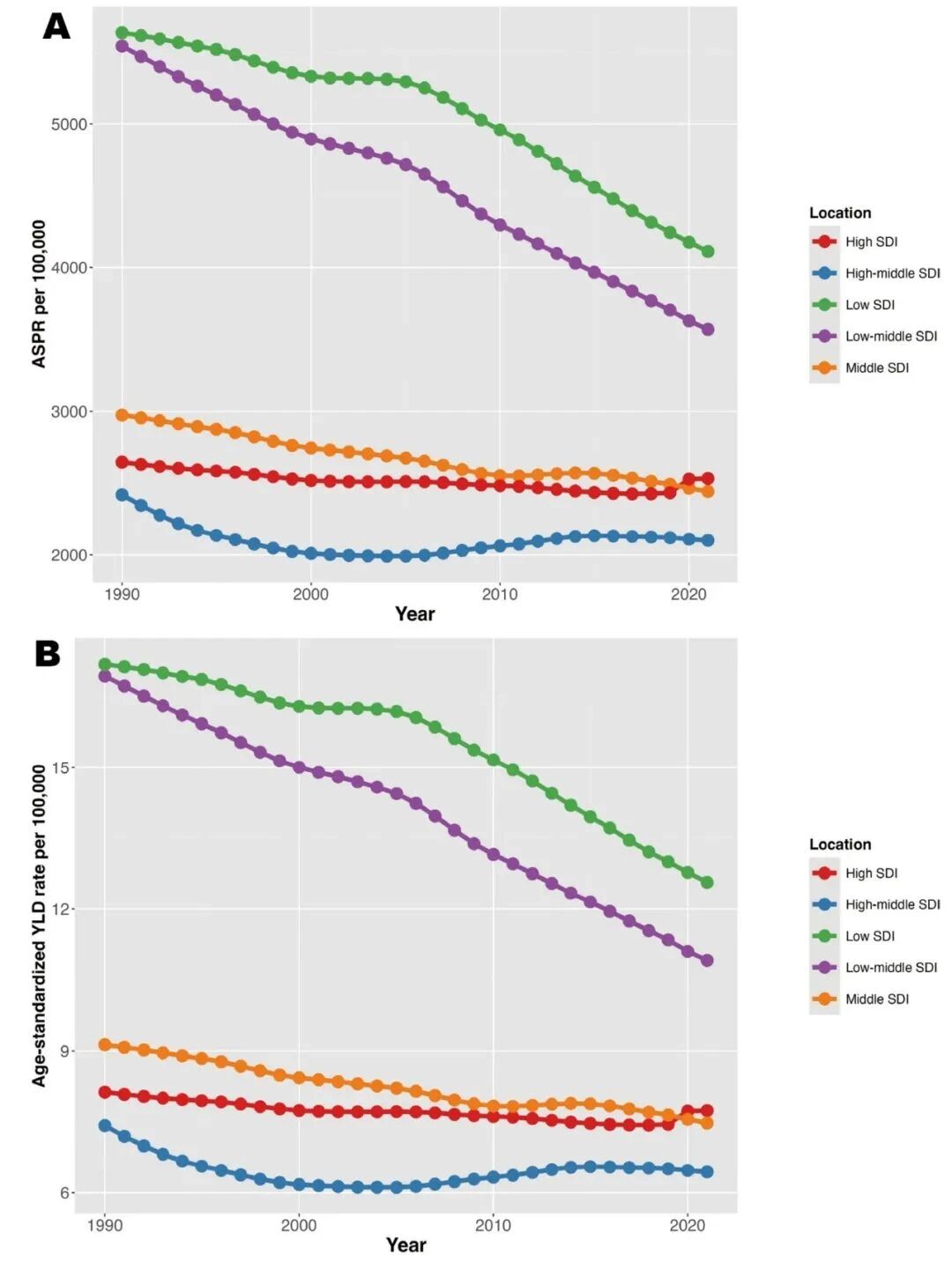
Figure 1. Age-standardized prevalence rates (A) and YLD trends (B) of POP across quintiles of SDI. SDI: Socio-demographic Index; ASPR: age-standardized prevalence rate; YLD: years lived with disability.
Regional burden of POP
At the regional level, the estimated age-standardized burden of POP was lowest in high-income Asia Pacific and highest in sub-Saharan Africa (Figure 2A). In 2021, the highest age-standardized prevalence rates were in sub-Saharan Africa (4420.9 per 100,000), Andean Latin America (4267.9 per 100,000), and South Asia (3757.2 per 100,000), while the lowest were recorded in high-income Asia Pacific (1081.3 per 100,000), East Asia (1651.3 per 100,000), and Southeast Asia (1598.6 per 100,000). Between 1990 and 2021, age-standardized prevalence increased only in two regions, Western Europe and Australasia, and decreased in most other regions. The largest declines were in South Asia (−41.3%, 95% UI −42.8% to −39.9%), Andean Latin America (−27.1%, 95% UI −30.5% to −23.4%), and Tropical Latin America (−26.3%, 95% UI −30.7% to −21.4%).
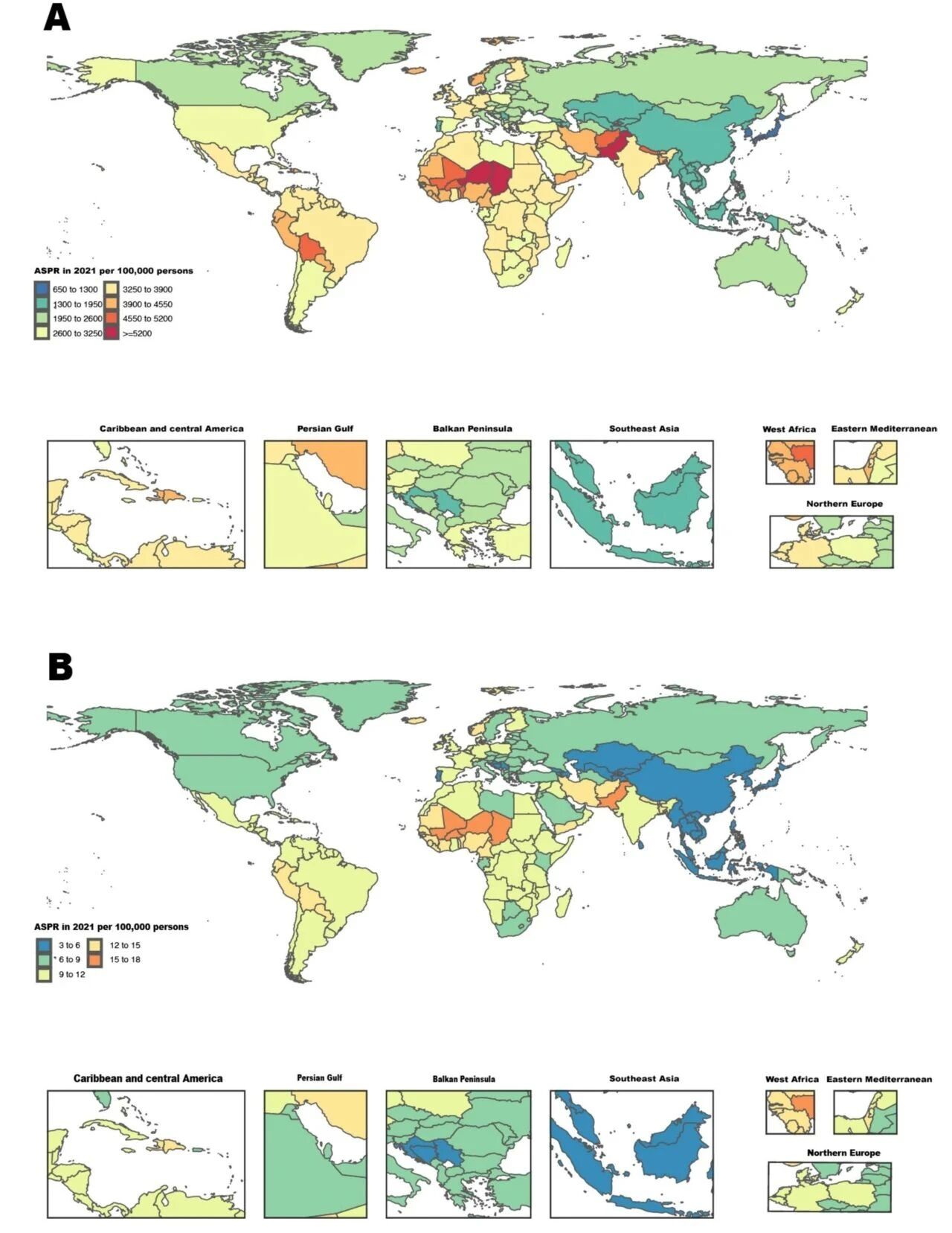
Figure 2. Age-standardized POP burden across 204 countries and territories in 2021. A: Global map of age-standardized prevalence rate; B: Global map of YLD.
From 1990 to 2021, regionally, SDI was negatively correlated with age-standardized YLD rates of POP within the same region. In low SDI regions (SDI ~0.3), age-standardized YLD rates peaked at nearly 20 per 100,000. YLD rates increased slightly with SDI up to about 0.5, then declined. In high SDI regions (SDI > 0.6), age-standardized YLD rates dropped to 5–10 per 100,000. Over 30 years, North Africa and Middle East, South Asia, Central Latin America, Tropical Latin America, Western Europe, the Caribbean, Andean Latin America, Western sub-Saharan Africa, and High-income North America had higher YLD rates than predicted by their SDI. In contrast, East Asia, Southeast Asia, Oceania, Central Asia, Eastern sub-Saharan Africa, and High-income Asia Pacific had lower burdens than expected (Figure 3).
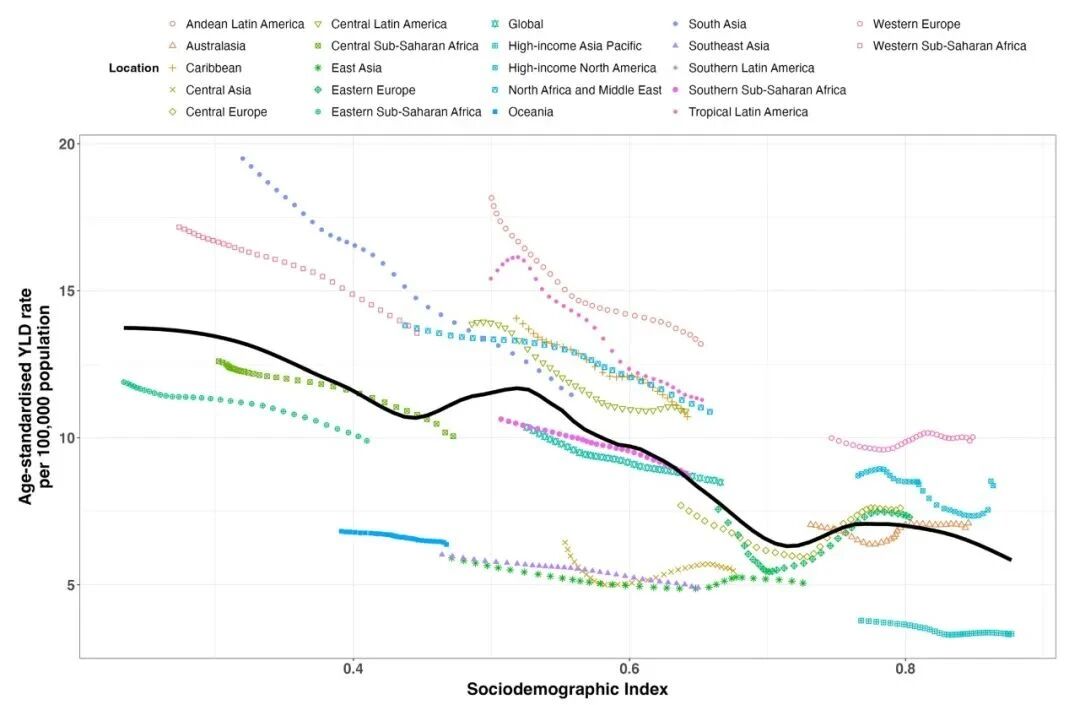
Figure 3. Age-standardized YLD rates of POP burden across 21 global regions by SDI from 1990 to 2021. For each region, 30 data points are plotted to show age-standardized YLD rates recorded during this period. Expected values based on SDI and incidence for all regions are shown as a solid line. Regions above this line, such as Andean Latin America, indicate a higher burden than expected. Conversely, regions like Southeast Asia had a lower burden than expected.
National burden of POP
In 2021, the three countries with the highest national age-standardized prevalence rates of POP were Niger (5633.3 per 100,000 women), Pakistan (5315.9 per 100,000 women), and Chad (5240.3 per 100,000 women). In contrast, Japan (1040 per 100,000), Singapore (1163.5 per 100,000), and Korea (1183.6 per 100,000) had the lowest age-standardized prevalence rates. Compared to 1990, age-standardized prevalence increased in 16 countries and decreased in the other 188. The largest increases were in Poland (11.9% [95% UI 5.4–19.6]), Israel (7% [95% UI −2.2–15]), and France (6.5% [95% UI −1.4–14.4]). On the other hand, the largest decreases were in Bangladesh (−42.3% [95% UI −46.9 to −37.9]), Nepal (−50.9% [95% UI −55.6 to −45.9]), and Saudi Arabia (−42% [95% UI −47.3 to −35.7]). Similar trends were observed for age-standardized YLD rates, consistent with national age-standardized prevalence rates.
At the national level from 1990 to 2021, a non-linear U-shaped relationship was found between SDI and age-standardized YLD rates for POP. In low SDI regions, age-standardized YLD rates peaked at nearly 20 per 100,000 (at approximately 0.2 on the SDI scale). As SDI increased, age-standardized YLD rates declined, reaching a minimum at around 0.7 on the SDI scale. Thereafter, YLD rates increased exponentially with further rises in SDI. Countries in low SDI regions such as Niger, Pakistan, Chad, and Nepal, as well as countries in high SDI regions such as Iceland, Norway, and Denmark, had burdens much higher than expected. In contrast, countries such as Japan, Singapore, Thailand, and Somalia had burdens significantly lower than expected.
Age-specific burden of POP
In 2021, the prevalence of POP showed an S-shaped distribution across age groups globally, peaking in the 80+ age group (11425.2/100,000), while the YLD rate was highest in the 75–79 age group (32.73/100,000). The age group 55–59 had the highest number of cases and YLDs, with 16.8 million prevalent cases and 52,000 YLDs. Notably, the prevalence and YLD rates of POP were significantly higher in those under 40 years old and remained relatively stable in those aged 65 and above. POP prevalence declined across all age groups between 1990 and 2021. Furthermore, regions with higher SDI had a higher proportion of middle-aged and older adults (>65 years) affected by POP.
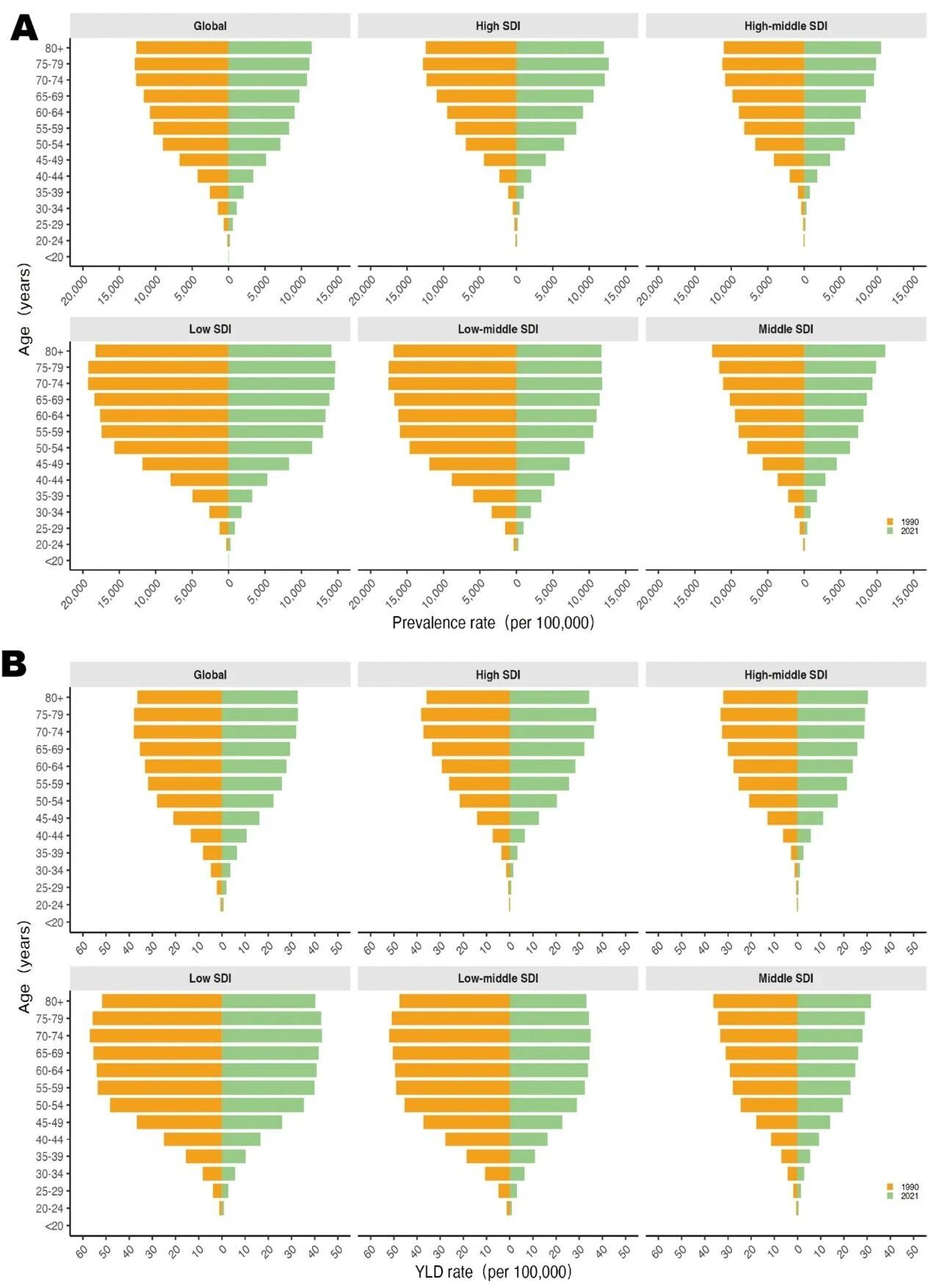
Figure 4. POP prevalence and YLDs by age group and SDI region in 1990 and 2021. A: Prevalence by age group and SDI region in 1990 and 2021; B: YLD rates by age group and SDI region in 1990 and 2021.
Global burden of POP projections
Using the Bayesian age-period-cohort (BAPC) model, we project that both the age-standardized prevalence rate and age-standardized YLD rate of POP will decline between 2022 and 2036. By 2036, the global prevalence of POP is expected to reach 156 million, a 25% increase from 2021. The average incidence of POP is projected to be 2554.12 per 100,000, a 7.8% decrease from 2021. The age-standardized YLD rate is projected to be 7.78 per 100,000. The shaded areas in the figures indicate potential fluctuations in ASPR and YLD rates, with annual changes up to 1%.
Conclusion
The global burden of POP decreased between 1990 and 2021, but the age-standardized prevalence remains high in low SDI regions. With an aging population, POP will continue to pose a significant burden on women’s health and socioeconomic systems. Strengthening global surveillance and prevention efforts for POP remains a critical challenge.
Expert Commentary
Pelvic organ prolapse (POP) is a common pelvic floor dysfunction disorder that severely affects the health and quality of life of women worldwide. Due to weakening of the pelvic support structures, pelvic organs such as the uterus, vaginal walls, rectum, and bladder may descend into the vagina or even protrude outward, causing a range of clinical symptoms including vaginal wall prolapse, uterine prolapse, defecation difficulties, and urinary abnormalities. With the acceleration of global population aging, POP has become an increasingly serious public health issue. It not only impairs patients’ physical health, leading to symptoms such as urinary incontinence, voiding difficulties, and sexual dysfunction, but also negatively impacts patients’ social, occupational, and emotional lives, causing psychological problems such as embarrassment, anxiety, and depression. Particularly in economically underdeveloped regions, women often face greater economic pressure and sociocultural constraints, making the burden of POP even heavier.
Despite the continuously rising prevalence of POP, global epidemiological research on it remains insufficient. This research gap partly stems from regional differences in socioeconomic conditions, cultural attitudes, and diagnostic criteria. Prevalence rates based on pelvic examination have been reported as high as 50%, but the incidence of symptomatic POP is generally lower, estimated between 3% and 6%. However, in economically impoverished areas, the actual prevalence may be much higher than reported in existing studies. Considering the trend of population aging, the prevalence of POP is expected to increase significantly in the future. For example, in the United States, the number of women affected by POP is projected to increase by 46% by 2050. This growth will place enormous pressure on healthcare systems and socioeconomic resources.
Currently, clinical management of POP primarily focuses on pelvic tissue repair after disease onset, including pelvic floor muscle training, pessaries, electrical stimulation, and surgical intervention. However, the importance of early assessment and prevention is increasingly recognized. In recent years, some researchers have developed prediction models and scoring systems aimed at identifying high-risk patients to prevent or delay the occurrence and progression of POP. For example, prediction models constructed using indicators such as age, parity, serum calcium, and 25-(OH)D3 can better guide clinical decisions, thereby improving the health of postmenopausal women. Timely intervention and early identification of risk factors are crucial for delaying the onset and progression of POP, improving women’s health, and reducing pressure on healthcare systems – these are also key goals for future public health initiatives.
The Global Burden of Disease (GBD) study project aims to assess the impact of various diseases, injuries, and related risk factors on global health. Although some studies have conducted comprehensive analyses using GBD 2019 data, no study has yet modeled or projected the future burden of POP. Therefore, this study uses GBD 2021 data to comprehensively examine the impact of POP at global, regional, and national levels, and applies the Bayesian age-period-cohort (BAPC) model to project the burden of POP over the next 15 years. By analyzing trends in age-standardized prevalence rates and years lived with disability (YLD) rates, it aims to provide important information for future healthcare planning and policy interventions, thereby more effectively addressing the growing burden of POP and improving the health and well-being of women globally.

