Guideline and Consensus | Expert Consensus on Diagnosis and Rehabilitation Treatment of Pelvic Floor Dysfunction (2024)
In 2024, numerous pelvic floor rehabilitation experts, based on clinical practice and scientific research, jointly developed more rigorous and scientific treatment guidelines and consensus. The emergence of these expert consensuses not only provides clinicians with more precise treatment guidance but also offers patients safer and more effective rehabilitation plans. At the same time, it marks the gradual progression of China’s pelvic floor rehabilitation field towards a standardized and normalized development path.
Methodology for Consensus Development

This consensus was developed following the items of the Appraisal of Guidelines for Research & Evaluation Ⅱ (AGREE Ⅱ). Based on the quality and strength of evidence-based medicine, the Grading of Recommendations Assessment, Development and Evaluation (GRADE) system was used to grade the quality of evidence and the strength of recommendations. The quality of evidence was classified into four levels: “A, B, C, D”, and the strength of recommendations was classified into two levels: “strong recommendation” and “weak recommendation”. Each recommendation and its strength were ultimately determined through discussion by the expert consensus group.

Diagnosis
01 Medical History Taking and Physical Examination
Recommendation 1: Detailed medical history taking and physical examination are helpful for correctly assessing the disease and establishing a definite diagnosis. (Quality of Evidence: Level C; Strength of Recommendation: Strong)
Taking a medical history and understanding the patient’s symptoms are very important. First, obtain basic information such as name, gender, age, place of birth, ethnicity, marital status, employment status, education level, etc. Second, collect the chief complaint, history of present illness, past medical history, marital and reproductive history, personal history, family history, menstrual history, sexual history, recent medication use, psychological status, and medical humanities concerns.
02 Anorectal Manometry
Recommendation 2: Anorectal manometry helps assess anorectal sensory and/or motor function, detect anorectal functional abnormalities, and assists in deciding patient treatment plans. (Quality of Evidence: Level B; Strength of Recommendation: Strong)
03 Pelvic Floor Ultrasound
Recommendation 3: Pelvic floor ultrasound is an important examination for diagnosing pelvic floor dysfunction. It allows static and dynamic observation of pelvic floor structures and muscle movement changes, enabling multi-level assessment of their function. It provides particularly comprehensive evaluation of levator ani and anal sphincter injuries, offering objective indicators for clinical diagnosis and treatment efficacy assessment. (Quality of Evidence: Level B; Strength of Recommendation: Strong)
04 Defecography
Recommendation 4: X-ray defecography is an important evaluation method for conditions such as outlet obstruction constipation and pelvic organ prolapse. However, it has limitations due to radiation exposure and relatively complicated procedure. (Quality of Evidence: Level A; Strength of Recommendation: Weak)
Recommendation 5: Ultrasound defecography offers advantages such as simple operation, good tolerability, and avoidance of radiation exposure. It can be used to evaluate pelvic floor dysfunction, especially outlet obstruction constipation. (Quality of Evidence: Level B; Strength of Recommendation: Weak)
Recommendation 6: Magnetic resonance defecography can be used to evaluate pelvic floor dysfunction, particularly posterior pelvic organ prolapse. However, its clinical application is limited by high cost and long examination time. (Quality of Evidence: Level B; Strength of Recommendation: Weak)
05 Colonic Transit Test
Recommendation 7: The colonic transit test is key to distinguishing different types of constipation. (Quality of Evidence: Level B; Strength of Recommendation: Weak)
06 Urodynamic Study
Recommendation 8: Urodynamic studies are of significant value in the diagnosis of stress urinary incontinence, but their utility for diagnosing pelvic organ prolapse requires further validation through high-quality, large-scale studies. (Quality of Evidence: Level B; Strength of Recommendation: Weak)
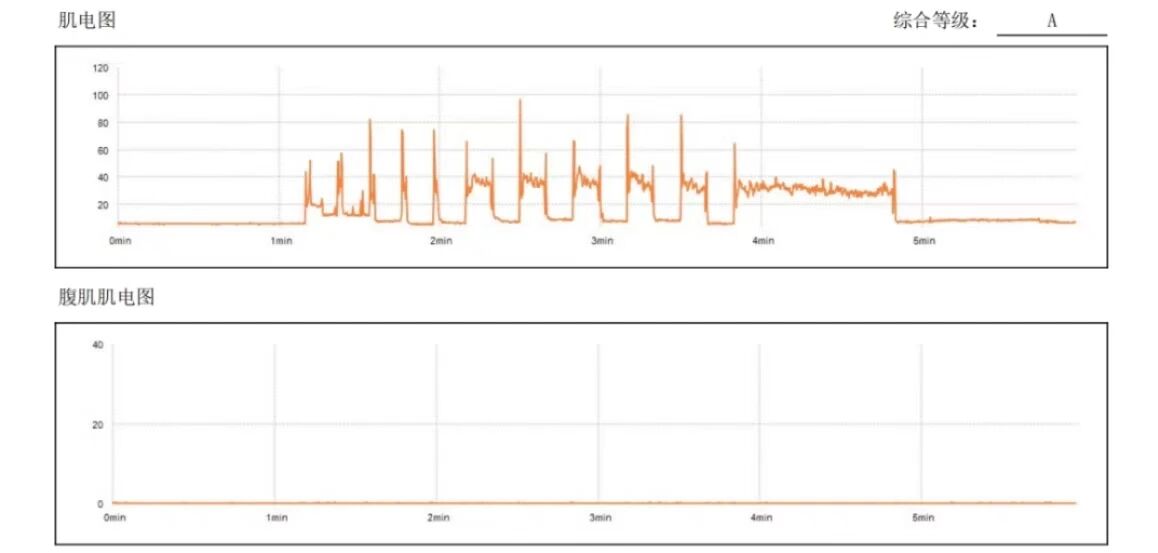
07 Pelvic Floor Electromyography Assessment
Recommendation 9: The Glazer protocol for pelvic floor surface electromyography is an important method for evaluating pelvic floor muscle function, especially for postpartum pelvic floor assessment. (Quality of Evidence: Level B; Strength of Recommendation: Strong)
Rehabilitation Treatment
01 Lifestyle Intervention
Recommendation 10: Lifestyle intervention is simple to perform and can be done anytime, making it the first-line treatment for patients with mild PFD. However, once a person’s lifestyle is established, it is difficult to change without limitations. Therefore, this method has considerable randomness, cannot be quantitatively evaluated or monitored, and its efficacy varies from person to person. (Quality of Evidence: Level B; Strength of Recommendation: Strong)
02 Biofeedback Therapy
Recommendation 11: Biofeedback therapy is a treatment method that requires active patient participation. It uses visual signals to reflect muscle activity information, fully utilizing the patient’s initiative. It is not only economical, convenient, and less painful but also has high patient acceptance. (Quality of Evidence: Level A; Strength of Recommendation: Strong)
03 Sacral Neuromodulation
Recommendation 12: Sacral neuromodulation has certain therapeutic effects on pelvic pain syndrome, neurogenic lower urinary tract dysfunction, interstitial cystitis, and chronic functional constipation. (Quality of Evidence: Level A; Strength of Recommendation: Strong)
04 Transcutaneous Electrical Stimulation
Recommendation 13: Transcutaneous electrical stimulation is inexpensive, safe, non-invasive, easy to learn, and allows adjustable stimulation current frequency and intensity, facilitating personalized treatment plans that are easily adopted by both patients and physicians. (Quality of Evidence: Level A; Strength of Recommendation: Strong)
05 Pelvic Floor Magnetic Stimulation
Recommendation 14: Magnetic stimulation therapy is characterized by simple operation, non-invasiveness, no penetration, and strong penetration ability. It can effectively improve pelvic floor function and has significant value for clinical promotion and application. (Quality of Evidence: Level A; Strength of Recommendation: Strong)

06 Oral Chinese Herbal Medicine
Recommendation 15: Oral administration of Chinese herbal decoctions has certain efficacy in improving pelvic floor dysfunction. However, due to large individual differences and low reproducibility, there are difficulties in clinical research and widespread application. (Quality of Evidence: Level B; Strength of Recommendation: Strong)
07 External Chinese Herbal Therapy
Recommendation 16: Traditional external Chinese herbal therapies include acupoint application, Chinese herbal enema, and Chinese herbal fumigation. These can serve as adjunctive therapies for patients with pelvic floor dysfunction and are worthy of clinical promotion and application. (Quality of Evidence: Level C; Strength of Recommendation: Weak) External Chinese herbal therapies include herbal fumigation, acupoint application, herbal enema, etc.
08 Acupuncture
Recommendation 17: Acupuncture therapy can be used as a primary treatment for PFD patients with various clinical manifestations. It can also be combined with medication or biofeedback therapy, offering advantages such as improved efficacy, shortened treatment duration, and reduced adverse reactions, with high value for clinical promotion and application. (Quality of Evidence: Level A; Strength of Recommendation: Strong) Acupuncture is an important component of traditional Chinese medicine and can comprehensively improve the various clinical manifestations of PFD, enhancing patients’ quality of life.
09 Other Traditional Chinese Medicine Therapies
Recommendation 18: Other TCM therapies such as press needles, acupoint injection, moxibustion, and tuina can serve as adjunctive therapies for treating PFD. When combined with other treatments, they help further improve clinical efficacy. (Quality of Evidence: Level C; Strength of Recommendation: Weak)
10 Psychological Intervention Therapy
Recommendation 19: In actual psychological intervention therapy, two-way communication should be established based on patient needs, and a specific psychological intervention plan should be implemented to help patients recover their health as soon as possible. (Quality of Evidence: Level B; Strength of Recommendation: Strong) Pelvic floor dysfunction often brings various negative emotions, such as anxiety, depression, and low self-esteem. Psychological intervention is one of the important means to treat pelvic floor dysfunction and improve patients’ quality of life. Common psychological intervention methods include cognitive behavioral therapy, mindfulness practice, and detached emotional therapy. The focus of these interventions is to help patients break free from negative thoughts and emotions, stimulate their active, positive concepts and self-regulatory behavioral abilities, learn better ways to deal with pain and discomfort, thereby reducing psychological stress and restoring quality of life.
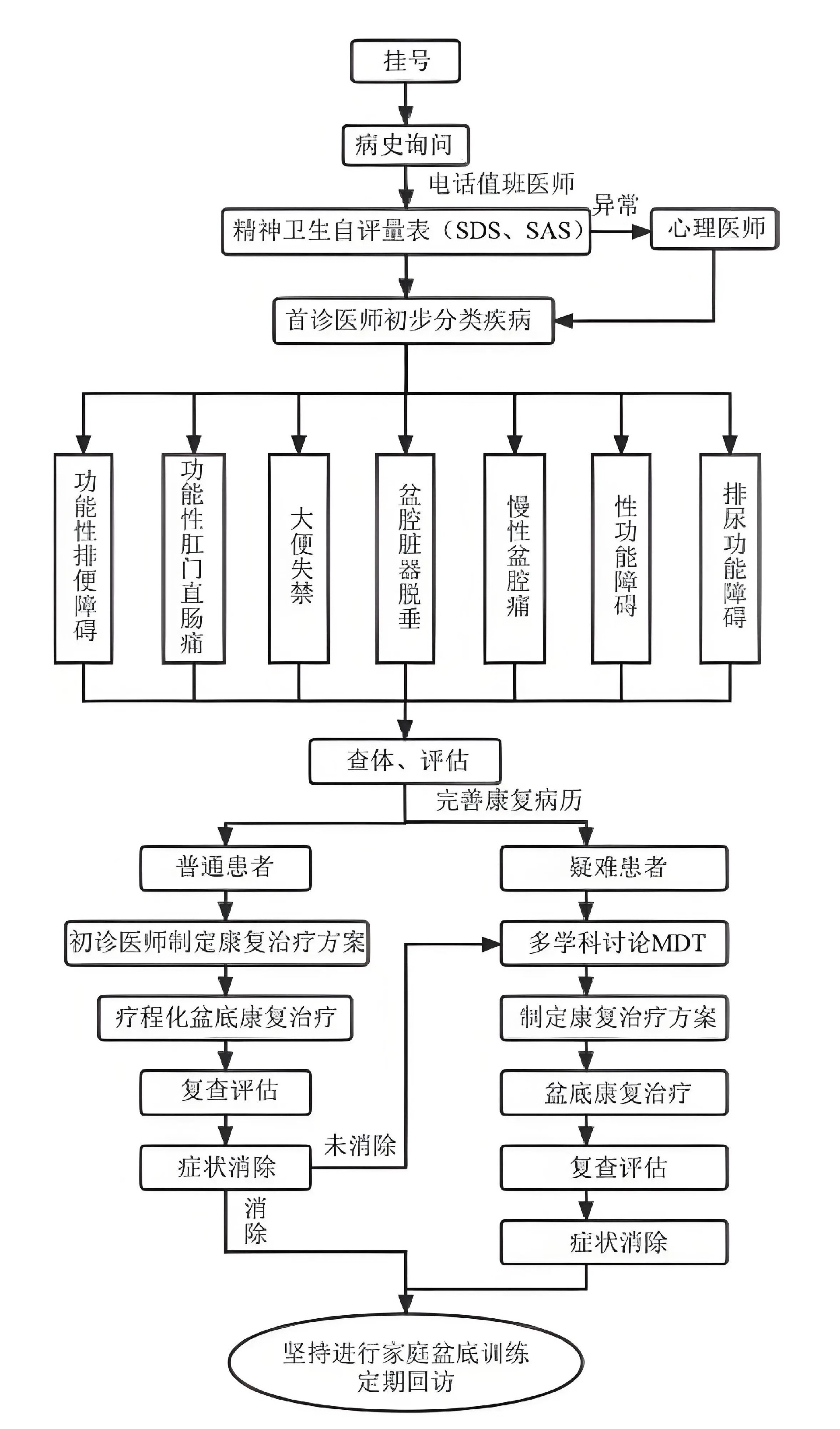
One-Stop Pelvic Floor Rehabilitation Diagnosis and Treatment
In recent years, some medical institutions have begun to explore the establishment of multidisciplinary pelvic floor centers. Many places have successively set up integrated pelvic floor diagnosis and treatment centers, integrating specialists from colorectal surgery, gynecology, urology, psychology, rehabilitation, and other departments to provide unified treatment for PFD patients.
Conclusion
The diagnosis and rehabilitation of pelvic floor dysfunction emphasize multidisciplinary collaboration, integrating comprehensive treatment from obstetrics and gynecology, urology, colorectal surgery, rehabilitation, and other specialties. At the same time, it requires physicians to have rich clinical experience and professional knowledge. Through this expert consensus, we hope to provide a reference for clinical practice, improve the diagnostic and therapeutic level of pelvic floor dysfunction, and bring better treatment outcomes and quality of life to patients. Clinical practice guidelines need to consider individual patient needs, local medical resources, and the specific characteristics of medical institutions. This consensus does not exclude the reasonableness of other interventions.

