Guideline Consensus | “Expert Consensus on the Individualized Optimized Diagnosis and Treatment Technology System for Pelvic Floor Dysfunction in Elderly Women” (2024)
Pelvic floor dysfunction (PFD) is a group of disorders characterized by the displacement of pelvic organs caused by various factors such as defects, weakness, injury, and dysfunction of the pelvic floor support structures, leading to pelvic organ prolapse (POP), urinary incontinence, sexual dysfunction, and other functional abnormalities of the pelvic organs. With the accelerating aging of the population in developed countries and China, PFD, which has a high incidence in elderly women, is one of the major diseases affecting women’s health.
There is a lack of large-scale epidemiological data on PFD in Chinese women. Some studies report that 45% of women in China suffer from varying degrees of PFD, with the incidence increasing with age. The incidence of urinary incontinence in women over 65 years old reaches 25%. With pregnancy, childbirth, the physiological process of aging, and exacerbated pathological damage, there is a functional disorder involving three systems: urinary, reproductive, and anorectal, including排尿, defecation, sexual dysfunction, and chronic pain.
This consensus, based on evidence-based evaluation of traditional diagnostic and therapeutic techniques combined with clinical management pathways, integrates current expert consensus on diagnostic and therapeutic techniques to propose an individualized optimized diagnosis and treatment plan. Optimizing the technical system for PFD in elderly women (aged ≥60 years) can improve the comprehensive intervention efficacy of PFD, optimize the quality of tiered medical care, and enhance the control rate of pelvic floor dysfunction without a significant increase in medical resource investment, which holds important clinical significance and social value.

I. Early Prevention and Control Protocol for Pelvic Floor Dysfunction
(1) Health Education
01 Pre-treatment Questionnaire
Includes understanding of the disease, its causes, influencing factors, treatment methods, efficacy evaluation, treatment adherence, and treatment schedule.
02 Education during Treatment
Provide one-on-one nursing guidance to patients receiving treatment, explaining pelvic floor muscle training methods.
03 Post-treatment Follow-up
Evaluate the effectiveness of biofeedback therapy, determine the interval for subsequent treatment, and regularly follow up for feedback information. Simultaneously, explain to patients the factors affecting treatment outcomes, including increased abdominal pressure, control of urinary tract infections, avoidance of heavy lifting, smoking and alcohol cessation, etc.
(2) Lifestyle Interventions
Smoking cessation, moderate exercise, nutritional management (avoiding hyperlipidemia), body weight control (18.5 kg/m² < BMI < 25 kg/m² is recommended), management of chronic diseases related to PFD (hypertension, diabetes, etc.), and treatment of conditions that increase abdominal pressure, such as long-term constipation and chronic cough.
Recommendation 1: The occurrence of PFD is closely related to personal lifestyle behaviors and chronic disease management. Medical staff at all levels should do their best to disseminate disease knowledge and ensure that recipients fully understand it, which is of great significance for primary and secondary prevention of the disease. Guiding individuals at risk to correct modifiable risk factors is important for controlling disease progression.
(3) Active Pelvic Floor Muscle Exercise
For patients with mild to moderate stress urinary incontinence (SUI) or mixed urinary incontinence, pelvic floor muscle training as first-line therapy should last at least 3 months.
Vaginal relaxation syndrome is an early manifestation of POP and requires early identification and intervention. For patients with symptoms of vaginal laxity, standardized active pelvic floor muscle training, manual therapy, and physical energy rehabilitation therapy are recommended.
Pelvic floor muscle training protocol: Sustain pelvic floor muscle contraction (i.e., Kegel exercises) for no less than 3 seconds, relax for 2-6 seconds, repeat continuously for 15-30 minutes, three times daily; or perform 150-200 Kegel exercises per day. Continue for 3 months or longer.
(4) Vaginal Cones (Vaginal Rehabilitation Device) Training to Enhance Active Pelvic Floor Muscle Training
When using, start with the lightest cone, insert it into the vagina and retain for 15-20 minutes. Once it can be comfortably retained, gradually switch to a heavier cone. After each weight increase, gradually add activities such as squatting, coughing, and jumping to progressively increase training difficulty and intensity.
(5) Pelvic Bioelectrical Stimulation Therapy
01 Indications
Vaginal laxity, SUI, overactive bladder (OAB), chronic pelvic pain (CPP).
02 Protocol
Electrical stimulation used in pelvic floor rehabilitation typically has a frequency ≤ 100 Hz. Based on the different effects of different frequencies, a clinical distinction is made: frequencies below 20 Hz are considered low frequency and are used to treat overactive muscles, while 50 Hz is considered high frequency and is used to treat relaxed muscles.
03 Frequency selection for different conditions
(1) Muscle contraction: Currents of 1-10 Hz can cause single muscle twitches, 25-50 Hz can cause complete muscle contraction, while 100 Hz can weaken or eliminate muscle contraction. Therefore, 50 Hz is generally chosen for strength training, and 20-30 Hz for endurance training.
(2) OAB: Currents of 5-20 Hz inhibit bladder contraction via the pudendal-to-hypogastric nerve reflex. The optimal frequency for bladder inhibition is 10 Hz.
(3) CPP: Includes transcutaneous and intravaginal protocols. Transcutaneous electrical nerve stimulation (TENS): frequency 100 Hz, pulse width 100-250 μs; Intravaginal electrical stimulation: frequency 5-20 Hz, to relieve overactive pelvic floor muscles.
(6) Magnetic Stimulation Therapy
Magnetic stimulation therapy is divided into pelvic floor stimulation mode and sacral nerve stimulation mode. Magnetic stimulation can continuously change frequency. The intensity of frequency conversion treatment should be adjusted to achieve a clear sensation of contraction and comfort for the patient.
01 Pelvic Floor Stimulation Mode
Includes understanding of the disease, its causes, influencing factors, treatment methods, efficacy evaluation, treatment adherence, and treatment schedule.
02 Sacral Nerve Stimulation Mode
Can be used for lower urinary tract dysfunction, defecation dysfunction, CPP, chronic prostatitis, pediatric enuresis, and other conditions.
Recommendation 2: Pelvic floor muscle training is divided into active muscle exercise and passive muscle training. Guiding women to perform correct pelvic floor muscle exercises, starting proper use of vaginal cones after achieving vaginal muscle strength of grade 3, and maintaining long-term adherence as much as possible is of great significance for the prevention and treatment of pelvic floor diseases. Additionally, if supplemented with passive muscle training modes such as necessary pelvic floor electromagnetic therapy and periodic assessments, the treatment effect will be enhanced.
(7) Laser and Radiofrequency Energy Device Therapy
01 CO2 Fractional Laser, Er:YAG Fractional Laser
Indications: vaginal laxity, SUI, genitourinary syndrome of menopause (GSM), etc.
02 Radiofrequency
Medical non-ablative radiofrequency can be divided into monopolar, bipolar, fractional, and hybrid systems, typically using low-temperature cooling.
Recommendation 3: Based on short-term clinical study reports, energy-based devices have a good safety profile, but long-term vulvovaginal sequelae are not yet known. Therefore, only through rigorously designed controlled studies with large sample collection can definitive conclusions about treatment safety be drawn.
(8) Pessary Therapy
Pessaries, depending on their functional design, are a first-line non-surgical treatment for uterine prolapse and SUI.
Recommendation 4: Patients should be fully informed about pessaries as a first-line conservative treatment for uterine prolapse and SUI. Proper trial fitting, education, guidance, and follow-up can greatly increase the success rate of conservative treatment, reduce unnecessary surgical treatment and economic expenditure, which is particularly important for primary care settings.
(9) Myofascial Manual Therapy
Pelvic floor myofascial manual therapy involves applying pressure and stretching to muscles with myofascial trigger points, releasing the tight bands and trigger points, relieving fascial restrictions, reducing pain sensitivity, relaxing spasmodic and painful muscle fascia, restoring blood supply, awakening proprioception of the pelvic floor muscles, inducing voluntary contraction and relaxation of the pelvic floor muscles, thereby achieving pain relief and functional improvement.
Mainly indicated for: various types of pelvic floor muscle and fascia-derived pain and dysfunction, such as pelvic floor myofascial pelvic pain, OAB, constipation, dyspareunia, functional anorectal pain, etc.
Recommendation 5: Myofascial manual therapy has the most prominent requirement for individualization. Before treatment, a full assessment should be performed, indications confirmed, and informed consent obtained from the patient. During treatment, movements should be gentle, and the patient actively encouraged to cooperate. Post-treatment observation and follow-up are necessary. In cases of poor response, timely multidisciplinary case discussion should be conducted to identify deeper causes and better treatment options.
II. Pharmacological Therapy for Pelvic Floor Dysfunction
Pharmacological therapy focuses on urge urinary incontinence (UUI)/OAB and symptomatic pain relief for some CPP cases.
Pharmacotherapy for UUI/OAB is divided into two categories: anticholinergic agents and β3-adrenoceptor agonists. Anticholinergic agents currently approved by the U.S. Food and Drug Administration (FDA) are shown in Table 1; optional β3-adrenoceptor agonists are shown in Table 2.
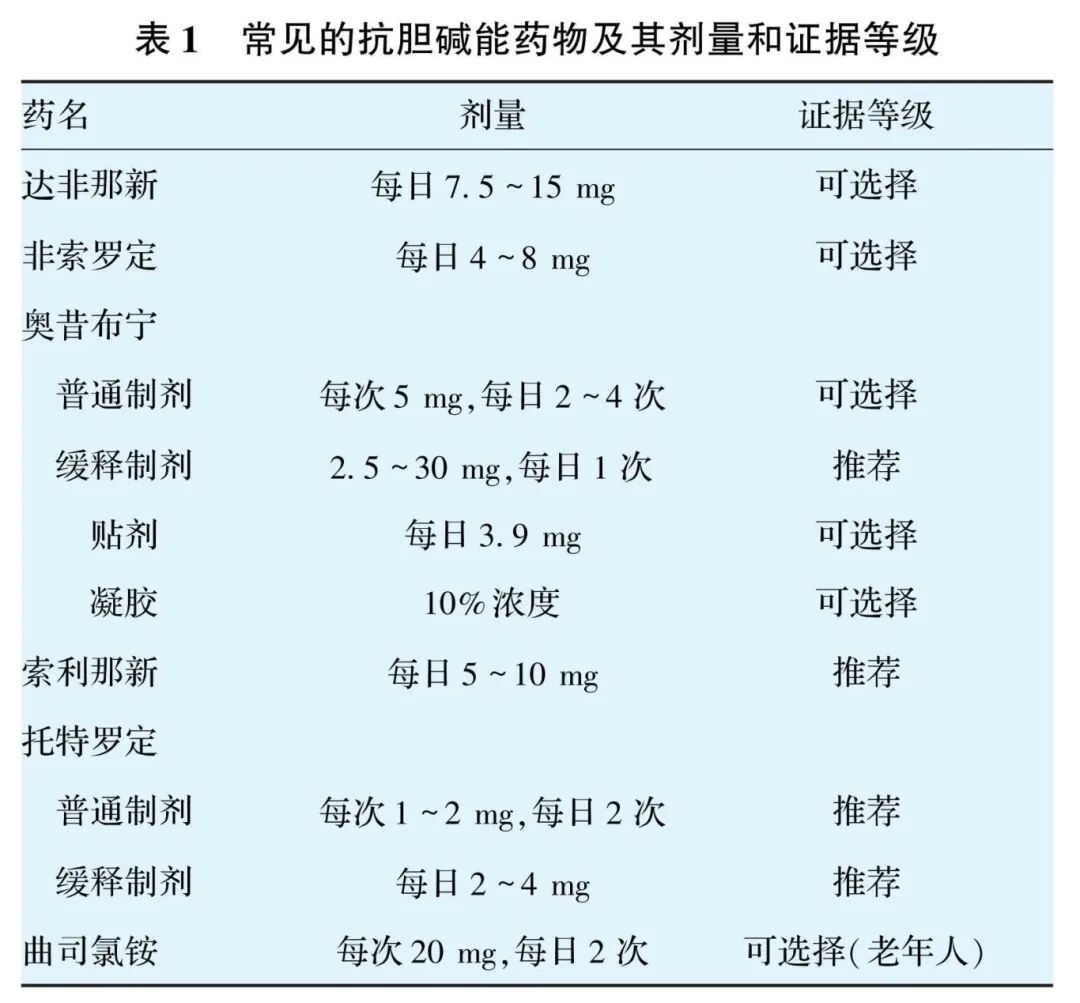

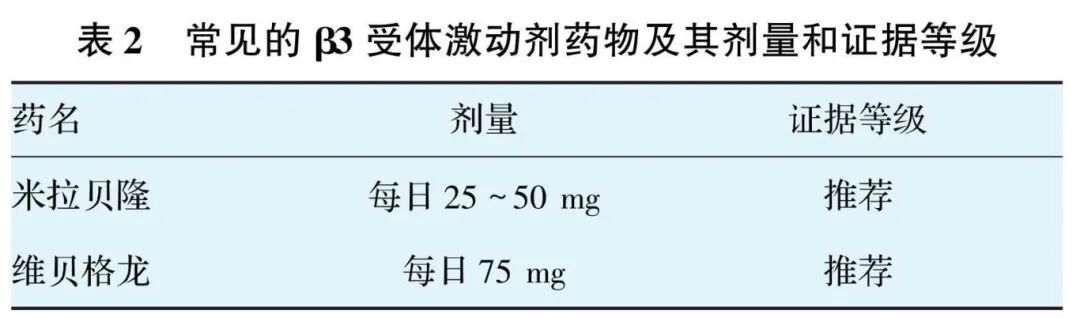
Recommendation 6: Pharmacological treatment of PFD mainly targets overactive bladder and the selection of local estrogen therapy for GSM, as well as symptomatic pain relief for CPP. At the same time, comprehensive assessment of the patient’s sleep and mental status is necessary. Combined medication, when needed, can achieve better therapeutic outcomes.
III. Individualized Surgical Plan
(1) Basic Principles
Conservative and non-surgical treatment options should be the first choice for POP (especially in young women). When making decisions about surgical treatment, special attention should be paid to the following points:
1. Anatomical restoration of the pericervical ring or vaginal apex.
2. Accurate preoperative multi-compartment assessment.
3. Postoperative attention to correcting obesity, chronic constipation, cough, and other issues that increase abdominal pressure.
(2) POP Surgical Procedures
Factors to consider when choosing a surgical approach generally include vaginal and abdominal procedures. The final procedure should consider:
1. The site and severity of prolapse.
2. Clinical signs (presence of voiding, defecation, sexual dysfunction, etc.).
3. The patient’s own physical condition.
4. Patient preference and the surgeon’s skill.
Recommendation 7: Based on the general principles of POP surgical treatment, emphasis is placed on customizing individualized treatment plans. In light of the FDA’s withdrawal of vaginal mesh and the difficulty and relatively long learning curve of transvaginal mesh pelvic floor reconstruction surgery, when surgery involving artificial mesh is considered, special care must be taken to communicate the pros and cons of the surgery thoroughly with the patient and obtain full informed consent. Surgeons should undergo specialized training and be authorized before performing such surgeries. Multidisciplinary discussions should be actively conducted when necessary to obtain the best treatment plan.
IV. Management of Surgical Complications
(1) Management of Complications of Pelvic Floor Reconstruction Surgery
Principles for managing mesh-related complications in POP reconstruction surgery are shown in Table 3.
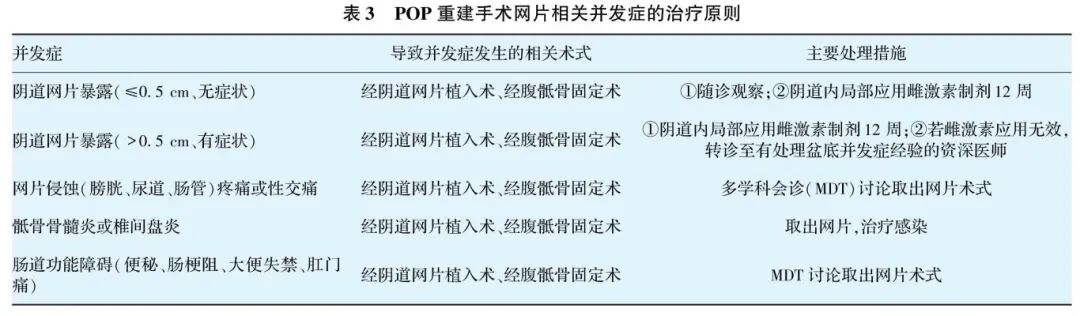
(2) Principles for Managing Complications Related to Tapes in Incontinence Surgery
Shown in Table 4.
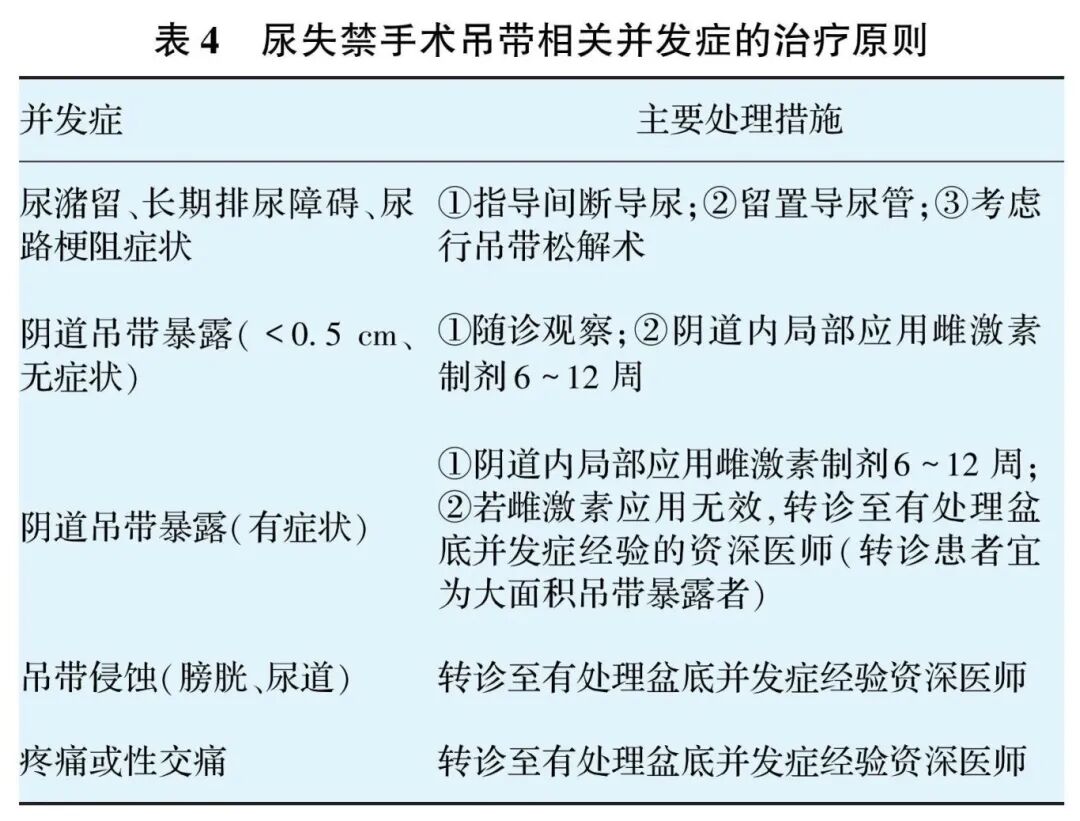

Recommendation 8: When surgical complications occur, physicians should actively communicate with the patient and manage the situation appropriately, initiating multidisciplinary discussions as early as necessary. The surgeon should be capable of managing complications, balancing the timing of conservative treatment and re-operation, and proactively registering complications. It is currently recommended to use the standardized terminology and classification system for complications related to implanted materials in female pelvic floor repair surgery published in 2011 by the International Urogynecological Association (IUGA) and the International Continence Society (ICS) Standardization of Terminology Committee for coding complications.
V. Surgical Treatment of Pelvic Organ Prolapse with Stress Urinary Incontinence
Recommendation 9: For POP with prolapse degree ≤ Stage II combined with mild to moderate SUI, conservative treatment is the first choice. For Stage III or IV POP combined with SUI, concurrent anti-incontinence surgery is recommended.
VI. Surgical Treatment of Pelvic Organ Prolapse with Occult Stress Urinary Incontinence (OSUI)
Recommendation 10: For severe POP combined with mild OSUI, POP surgery can be performed first, followed by close follow-up. If de novo SUI does occur, SUI surgery can be performed 6 months after the initial surgery after obtaining full informed consent from the patient. For severe POP combined with moderate to severe OSUI, the decision to perform concurrent SUI surgery should be made after thorough doctor-patient communication.
VII. Management of Surgical Recurrence
Recommendation 11: Treatment after recurrence emphasizes a comprehensive evaluation as if treating prolapse for the first time, actively engaging multidisciplinary discussions to determine the most appropriate management plan, and providing health guidance and lifelong follow-up.

